Table of Contents
ToggleMastering medication administration is a daunting milestone for any aspiring healthcare professional, but this pharmacology study guide for nursing students is designed to alleviate that stress. Many learners struggle with the sheer volume of memorization required for clinical rotations and board exams. By focusing on core mechanisms rather than rote recall, you can transform your study sessions into a more efficient, evidence-based process. Much like the rigors of student research, mastering pharmacology requires a systematic approach to data analysis and application. When you view drug classes as scientific families rather than isolated facts, the complexity begins to dissolve into a logical, manageable framework.
This guide provides the one essential, unbeatable strategy to help you excel in your studies and ensure patient safety at the bedside, ultimately bridging the gap between classroom theory and the fast-paced reality of clinical practice.
Understanding Pharmacology Basics for Nursing Students
To build a solid foundation, you must first understand the fundamental language of medicine. This section clarifies how drugs interact with the body and why understanding nomenclature is crucial for safe practice.
Decoding Drug Nomenclature and Classifications
- Identify the difference between generic and trade names to prevent medication errors.
- Recognize prefixes and suffixes (e.g., “-olol” for beta-blockers) to categorize drugs instantly.
- Use established pharmacological databases to verify classifications during your student research projects.
How Pharmacodynamics Affect Clinical Outcomes
- Study the “lock and key” model of receptor binding.
- Understand the difference between agonists (which initiate action) and antagonists (which block action).
- Analyze how drug potency and efficacy impact patient symptom management.
The One Unbeatable Strategy: Prototype Drug Memorization
Relying on memory alone is a recipe for burnout in nursing school. Instead, focusing on prototype drugs allows you to understand entire families of medication through a single, representative example.
Why Prototypes are the Key to Clinical Pharmacology
- Use the prototype as a baseline to predict the effects of newer, similar drugs.
- Reduce cognitive load by learning the “model” drug thoroughly rather than memorizing every variant.
- Streamline your study time by focusing on the most commonly prescribed medications in clinical settings.
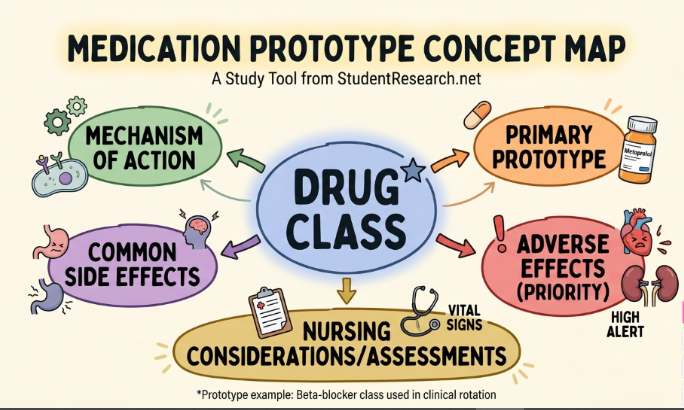
Grouping Medication Classes by Therapeutic Action
- Create classification charts based on the primary condition treated (e.g., pain, hypertension).
- Map out side effects and nursing implications for each therapeutic group.
- Apply the “prototype-first” method when reviewing your clinical case studies.
Essential Pharmacokinetics for Safe Medication Administration
Pharmacokinetics is the study of what the body does to the drug. Understanding these processes is vital for adjusting doses and timing for diverse patient populations.
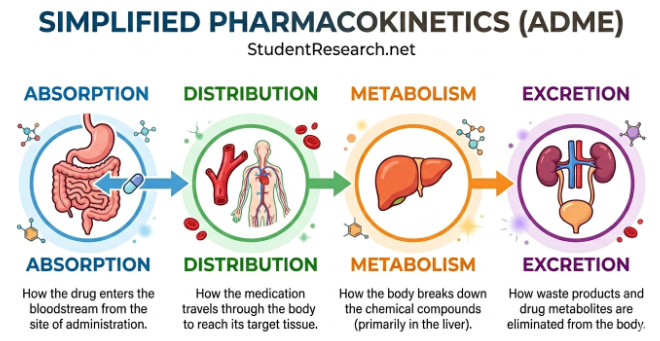
The ADME Principle: A Quick Review
- Absorption: How the drug enters the bloodstream from the site of administration.
- Distribution: How the medication travels through the body to reach its target tissue.
- Metabolism: How the liver processes and breaks down the chemical compounds.
- Excretion: How the kidneys or other pathways eliminate the drug from the body.
High-Yield Drug Classes Every Student Must Master
To excel in pharmacology, you must move beyond rote memorization and start understanding the therapeutic intent and clinical logic of drug families. Below, we explore three critical categories using structured prototype profiles to streamline your learning. To further assist with your academic success, refer to this comprehensive guide: Academic Writing Support Resources.
1. Antihypertensives: ACE Inhibitors and Beta-Blockers
ACE inhibitors and beta-blockers are foundational in treating cardiovascular disease. Their mechanism of action dictates how you monitor patients.
- Prototype Profile: Lisinopril (ACE Inhibitor)
- Indications: Hypertension, Heart Failure, and post-Myocardial Infarction.
- Mechanism: Inhibits the angiotensin-converting enzyme, preventing the conversion of Angiotensin I to Angiotensin II, which promotes vasodilation and lowers blood pressure.
- Contraindications: Pregnancy (teratogenic), history of angioedema, and renal artery stenosis.
- Side Effect Profile: Dry, persistent “ACE cough,” hyperkalemia, dizziness, and headache.
- Critical Nursing Assessments: Monitor potassium levels (do not administer if >5.0 mEq/L); assess for persistent cough; monitor BP before and after the first dose (risk of “first-dose hypotension”).
- Prototype Profile: Metoprolol (Beta-Blocker)
- Indications: Hypertension, Angina, and supraventricular arrhythmias.
- Mechanism: Selectively blocks Beta-1 receptors in the heart, slowing the heart rate and reducing myocardial contractility.
- Contraindications: Bradycardia, second or third-degree heart block, and cardiogenic shock.
- Side Effect Profile: Bradycardia, fatigue, mask signs of hypoglycemia in diabetics, and sexual dysfunction.
- Critical Nursing Assessments: Check apical pulse for one full minute prior to administration (hold if <60 bpm); educate patients not to stop abruptly to prevent rebound hypertension.
| Drug Class | Action | Key Nursing Priority |
| ACE Inhibitors | Vasodilation | Hyperkalemia monitoring |
| Beta-Blockers | Slows heart rate | Bradycardia monitoring |
2. Analgesics: Opioids and Non-Opioids
Managing pain safely requires a clear understanding of therapeutic ceilings and toxicity profiles.
- Prototype Profile: Morphine (Opioid)
- Indications: Severe acute, chronic, and cancer-related pain.
- Mechanism: Binds to mu-opioid receptors in the CNS, altering pain perception and emotional response to pain.
- Contraindications: Severe asthma, upper airway obstruction, and paralytic ileus.
- Side Effect Profile: Respiratory depression, sedation, constipation, nausea, and urinary retention.
- Critical Nursing Assessments: Perform respiratory assessment (hold if <12/min); ensure naloxone is readily available; implement a bowel regimen to counteract opioid-induced constipation.
- Prototype Profile: Acetaminophen (Non-Opioid)
- Indications: Mild to moderate pain and fever.
- Mechanism: Inhibits prostaglandin synthesis in the CNS; has antipyretic and analgesic properties but minimal anti-inflammatory effects.
- Contraindications: Severe hepatic impairment or active liver disease.
- Side Effect Profile: Generally safe at therapeutic doses; major risk is hepatotoxicity with overdose.
- Critical Nursing Assessments: Cap total daily dose at 3,000mg; screen for alcohol use; monitor liver function tests (LFTs) for long-term therapy.
| Analgesic | Primary Concern | Assessment Tool |
| Opioids | Respiratory Depression | Respiratory Rate/Sedation Scale |
| Non-Opioids | Hepatotoxicity | Liver Function Tests |
3. Antibiotics: Mechanisms and Spectrum of Activity
Successful antibiotic therapy relies on culture-guided selection and patient adherence to prevent resistance.
- Prototype Profile: Amoxicillin (Penicillin class)
- Indications: Broad-spectrum treatment for respiratory, ear, and urinary infections.
- Mechanism: Inhibits bacterial cell wall synthesis by binding to penicillin-binding proteins, leading to cell lysis.
- Contraindications: History of severe hypersensitivity/allergic reaction to penicillins or cephalosporins.
- Side Effect Profile: Diarrhea, rash, superinfection (e.g., vaginal yeast infections or C. diff).
- Critical Nursing Assessments: Ask about prior antibiotic allergies; monitor for signs of anaphylaxis (hives, wheezing); teach the patient to finish the entire course to prevent resistance.
| Antibiotic Type | Key Focus | Clinical Goal |
| Bactericidal | Kill bacteria | Eradication of infection |
| Bacteriostatic | Inhibit growth | Immune system clearance |
Mastering Medication Safety and Error Prevention
Clinical safety is the primary goal of every nurse. Implementing standardized protocols reduces the likelihood of “never events” and enhances patient outcomes by mitigating the risks associated with complex pharmacological interventions.
The “Human Factors” Analysis: Why Errors Occur
Medication errors are rarely the result of a single person’s mistake; they are typically the result of a “Swiss cheese” model where multiple systemic failures align.
- High-Pressure Environments: Rapid-paced clinical settings often lead to distractions during medication preparation, causing nurses to miss critical steps in the “five rights.”
- Fatigue and Burnout: Long shifts, particularly night shifts, impair cognitive function and reaction times, making it harder to detect subtle discrepancies in drug dosages or orders.
- Documentation Errors: Misinterpreting handwritten orders or failing to reconcile electronic health records (EHR) during patient handovers remains a leading cause of preventable harm.
- Workarounds: Shortcuts, such as pre-labeling syringes or bypassing barcode scanning systems, are often adopted to save time but ultimately destroy the safety barriers built into the system.
Identifying Look-Alike and Sound-Alike Medications
- The Tall Man Lettering System: Use mixed capitalization (e.g., DOPamine vs. DOBUTamine) to visually distinguish drugs that share similar spellings.
- Double-Check Protocols: Always perform an independent double-check for “High Alert” medications like Insulin, Heparin, and Chemotherapy agents.
- Scanning Technology: Utilize barcode medication administration (BCMA) systems to ensure you have the right patient, right dose, and right drug every time.
The “What Would You Do?” Clinical Scenario
Consider this common, high-stakes scenario: You are preparing to administer a scheduled dose of Warfarin (an anticoagulant) to a patient. Upon reviewing the patient’s updated medication list, you notice they were also just prescribed Ibuprofen for a headache by a consulting physician who was unaware of the patient’s current treatment.
Your Step-by-Step Nursing Process:
- Stop and Hold: Do not administer the Warfarin or the Ibuprofen until you have clarified the conflicting orders.
- Verify and Consult: Compare the orders with the patient’s chart and cross-reference the interaction in your facility’s clinical database.
- Collaborate: Use the SBAR framework to contact the primary provider or pharmacist. Explain that the interaction between the anticoagulant and the NSAID significantly increases the patient’s risk of gastrointestinal bleeding.
- Educate and Resolve: Once the provider clarifies the order, educate the patient on why they should not take OTC medications without nursing consultation.
- Document: Ensure the incident is clearly documented in the patient’s record, noting that you intercepted a potential adverse drug event to prevent patient harm.
By adopting a culture of “safety first,” you transform your clinical practice from simple administration to high-level advocacy, ensuring that your patients are protected from preventable harm.
Pharmacology Study Tips for Nursing School Exams
To reach a mastery level, you must transition from passive reading to active, data-driven study techniques. Your student research methodology should be applied to your own brain’s learning patterns.
Creating Effective Drug Flashcards using Spaced Repetition
- The Leitner System: Use a box with three compartments. If you get a card right, move it to the second compartment (review in 3 days). If wrong, keep it in the first (review daily).
- Card Anatomy: On the front, put the Drug Name and Class. On the back, include the “Big Three”: Mechanism, Primary Nursing Assessment, and the most dangerous side effect.
- Focus on Logic: Don’t just write “causes hypotension.” Write “causes hypotension -> check BP -> monitor for dizziness.”
Applying Active Recall for Long-Term Retention
- Concept Mapping: Instead of lists, draw a center bubble for “Hypertension” and branch out to ACE inhibitors, Beta-Blockers, and Diuretics. Note how they interact differently to achieve the same result.
- Peer Teaching: The best way to identify gaps in your student research is to attempt to teach a difficult drug class to a classmate. If you cannot explain the “why” behind the “what,” you need to review that section again.
- Digital Integration: Use tools like Lexicomp to quickly verify contraindications, but ensure you are documenting your learning process in your own words to avoid plagiarism and ensure deep understanding.
Clinical Pharmacology: Bridging Theory to Bedside
Theory provides the framework, but your clinical shifts provide the ultimate test of your pharmacological knowledge. To bridge the gap between textbook memorization and high-acuity bedside practice, you must learn to synthesize data rapidly. If you are struggling to structure your clinical observations or case studies during your rotations, I recommend utilizing this guide on Argumentative Research Paper Topics to refine your documentation and critical analysis skills, which are essential for academic nursing success.
Developing a Medication Action Plan for Patients
A robust action plan is more than just following the “Five Rights” of medication administration; it requires anticipating the patient’s physiological response to every intervention.
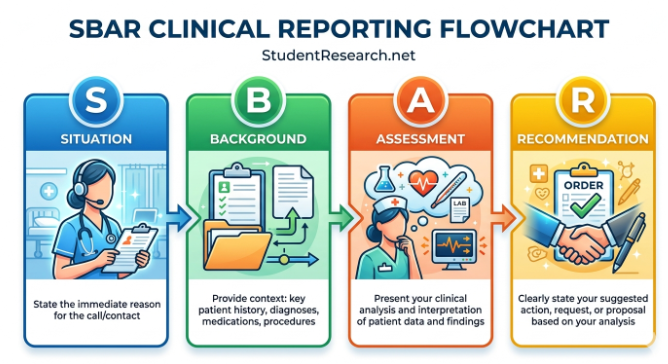
- The SBAR Framework: When you identify a potential drug-related issue, such as a contraindication or an adverse reaction, you must communicate it with precision. Using the SBAR tool ensures that your clinical reasoning is clear and actionable:
- Situation: State the patient’s current status (e.g., “Mr. Smith is scheduled for his 0900 dose of Furosemide”).
- Background: Provide relevant history (e.g., “He is currently experiencing muscle weakness and has a history of hypokalemia”).
- Assessment: Explain your clinical analysis (e.g., “His most recent potassium level is 3.1 mEq/L, which puts him at severe risk for cardiac arrhythmias if a loop diuretic is administered”).
- Recommendation: Offer a definitive solution (e.g., “I recommend we hold the Furosemide dose, notify the provider for potassium replacement, and re-draw the electrolyte panel”).
Monitoring Parameters: Moving Beyond Blood Pressure
Clinical assessment in pharmacology is multi-dimensional. You must look beyond simple vital signs and correlate medications with laboratory values and systemic organ function.
- Electrolyte Labs and Diuretics: For a cardiac patient on loop diuretics, monitoring blood pressure is only the baseline. You must consistently check electrolyte labs—specifically Potassium, Magnesium, and Sodium—before administration, as these drugs often cause significant electrolyte wasting.
- Renal and Hepatic Function: Many medications require dose adjustments based on the patient’s Creatinine Clearance (for kidney function) or AST/ALT levels (for liver function). If a patient is exhibiting signs of decreased urinary output, you must reassess whether the current drug dosage remains safe or if toxicity is a looming risk.
- Integrating Evidence-Based Data: Always cross-reference your patient’s specific lab values against your facility’s drug database, such as Lexicomp or UpToDate.
By consistently applying these diagnostic and communication frameworks, you transition from being a student who simply “passes” medications to a clinician who actively improves patient safety outcomes. Remember, every drug you administer is a clinical intervention that requires a complete cycle of assessment, action, and evaluation.
Conclusion: Mastering Your Nursing Pharmacology Journey
Consistency and a strategic approach are your best tools for success. Remember that mastering drug classes with this pharmacology study guide for nursing students will help you learn one essential and unbeatable strategy to pass your exams easily. By combining your classroom knowledge with active clinical application, you are not just memorizing lists—you are preparing to protect the health and safety of your future patients. Keep building your toolkit, stay curious, and continue refining your skills as you progress through your nursing education.