Table of Contents
ToggleBridging the Gap from Student to Professional Nurse
The transition from a classroom setting to the high-stakes environment of a hospital floor is one of the most pivotal moments in a healthcare career. Utilizing smart goals for nursing students during preceptorship examples allows you to transform overwhelming clinical shifts into a structured roadmap for professional excellence. By setting clear intentions, you move beyond mere observation and begin to master the art of critical thinking and hands-on patient care.
The Strategic Framework of SMART Goals in Clinical Practice
Setting objectives isn’t just about finishing a shift; it is about creating a measurable path toward becoming a licensed professional. This section explores why a structured framework is essential for navigating the complexities of modern healthcare environments. When students engage in active student research regarding their specific unit protocols, they can better align their personal growth with institutional standards.
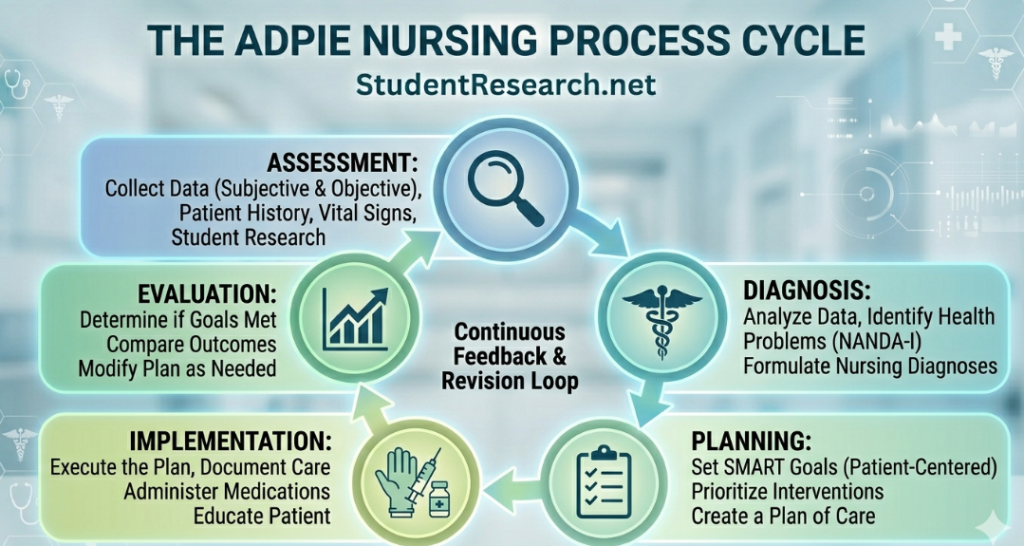
Breaking Down the SMART Acronym for Nursing Excellence
- Specific: Clearly define what clinical skill or knowledge area you intend to improve.
- Measurable: Determine the criteria you will use to track your progress throughout the rotation.
- Achievable: Ensure the goal is realistic given your current level of training and the unit’s resources.
- Relevant: Align your objectives with the core competencies required for your nursing degree.
- Time-bound: Set a specific deadline, such as the end of week four, to reach your milestone.
Why Specificity Prevents Clinical Errors
- Eliminates ambiguity in high-pressure situations like code blues or rapid responses.
- Focuses your preceptor’s feedback on distinct, actionable behaviors rather than generalities.
- Reduces cognitive load by narrowing your focus to one mastery area at a time.
Struggling to navigate the complex world of AI in nursing education? Ensure your clinical papers remain original and evidence-based with help from StudentResearch.net. Our experts provide ethical guidance on academic integrity and plagiarism management for nursing scholars.
Essential Performance Metrics: A Comparative Overview
Understanding where you stand compared to industry benchmarks can help you tailor your smart goals for nursing students during preceptorship examples. The following data highlights the common areas where students focus their development to meet entry-level professional standards. Comprehensive student research into these metrics helps bridge the gap between academic theory and the fast-paced reality of clinical rotations.
| Performance Metric | Student Average (Start) | Professional Benchmark | Improvement Strategy |
| Med-Pass Speed | 25 mins per patient | 10 mins per patient | Parallel preparation tasks |
| Documentation Accuracy | 70% error-free | 99% error-free | Real-time charting habits |
| Critical Thinking Index | Level 1: Reactive | Level 3: Proactive | Case study debriefing |
| Technical Skill Fluency | Requires 1:1 supervision | Independent with oversight | High-frequency repetition |
Top 31 High-Impact Preceptorship Goal Examples
Success in a clinical setting requires a diverse set of objectives covering everything from technical skills to emotional intelligence. Here are the 31 specific milestones you should aim to achieve during your transition to practice, ensuring you cover every facet of the nursing process.
Mastering Technical Proficiency and Hands-On Care
- #1: Perform five successful peripheral IV starts under supervision by the end of the second week.
- Focus on vein selection by palpating for “bounce” rather than relying on sight alone.
- Practice aseptic technique and ensure the stabilization of the catheter to prevent infiltration.
- Document the procedure, including the gauge used, the site location, and the patient’s tolerance of the event.
- Engage in student research regarding the latest infusion therapy standards to minimize complications like phlebitis.
- #2: Independently manage a Foley catheter insertion using a sterile technique by week three.
- Organize the sterile field on the bedside table before beginning the procedure to avoid contamination.
- Properly identify male vs. female anatomical landmarks to ensure correct placement on the first attempt.
- Maintain strict adherence to CAUTI (Catheter-Associated Urinary Tract Infection) prevention protocols.
- Verbalize each step of the sterile process to your preceptor to demonstrate cognitive mastery.
- #3: Demonstrate the correct “six rights” of medication administration for a full patient load.
- Verify the right patient, drug, dose, route, time, and documentation for every single pill or vial.
- Utilize the electronic MAR (Medication Administration Record) to cross-reference allergies and interactions.
- Perform a bedside education session for the patient regarding the purpose and side effects of their meds.
- #4: Conduct a comprehensive head-to-toe assessment in under 15 minutes by the midpoint of the rotation.
- Develop a systematic “top-down” approach so that no body system (neuro, cardiac, respiratory, GI/GU) is missed.
- Integrate skin checks and edema assessments while performing other tasks to increase efficiency.
- Communicate abnormal findings, such as new onset crackles or diminished pedal pulses, to your preceptor immediately.
- #5: Master the operation of PCA pumps and standard infusion devices used on the unit.
- Understand the safety limits and “hard stops” programmed into the facility’s smart pump library.
- Demonstrate the ability to troubleshoot common alarms, such as “occlusion upstream” or “air in line.”
- Independently perform a dual-nurse verification for high-alert medications like heparin or insulin.
Need a customized SBAR guide or a clinical prioritization hierarchy? Let StudentResearch.net design professional infographics and pharmacological study aids tailored to your rotation. We help nursing students transform complex clinical data into high-quality, visual learning tools today!
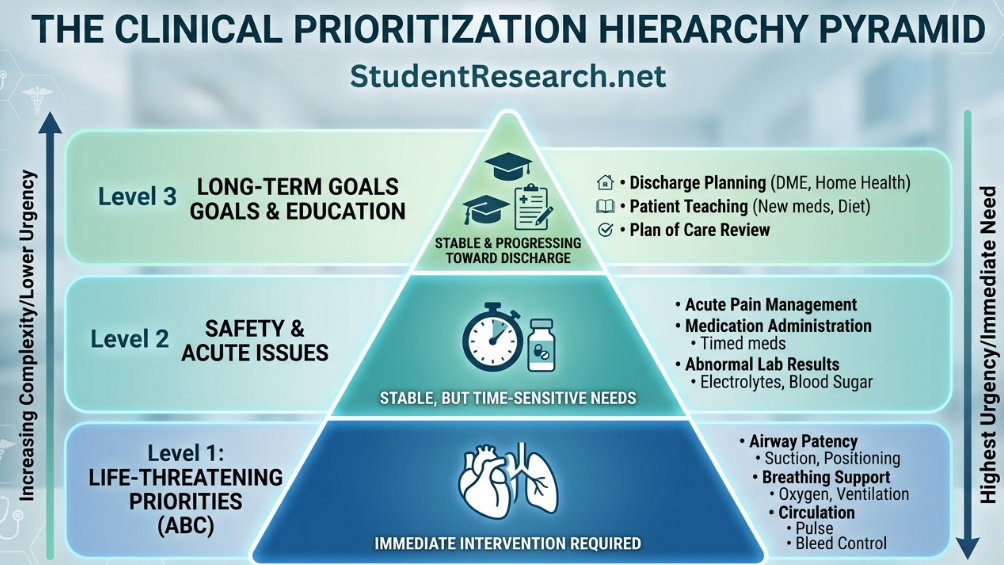
Critical Thinking and Prioritization Milestones
- #6: Correctly identify early signs of sepsis in a patient and report to the preceptor immediately.
- Monitor for the “Sepsis Trio”: altered mental status, increased respiratory rate, and low blood pressure.
- Correlate vital sign trends with laboratory data like elevated lactic acid or white blood cell counts.
- Prepare for the “Sepsis Bundle” interventions, including fluid resuscitation and early antibiotic delivery.
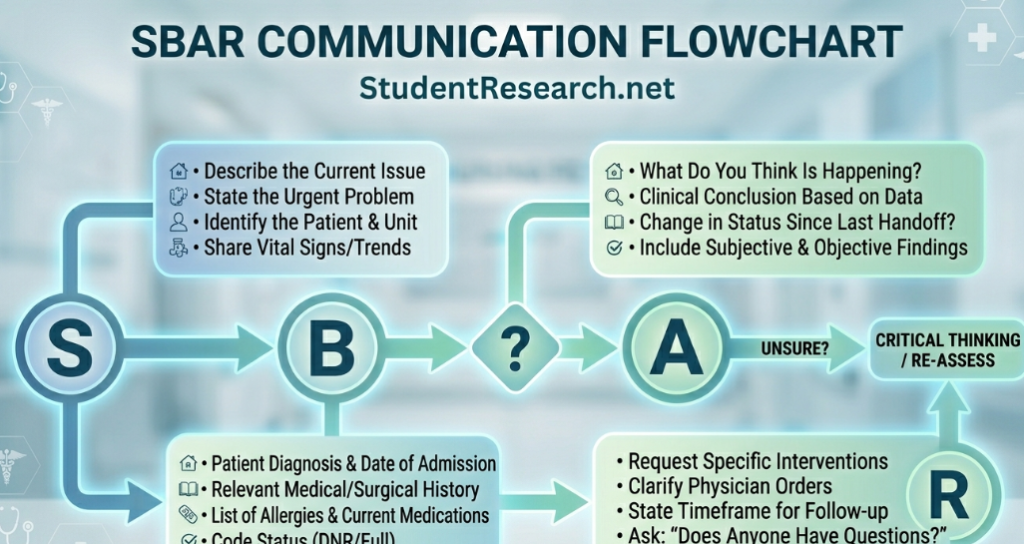
- #7: Utilize the SBAR communication tool for three physician notifications by week five.
- Situation: State the immediate reason for the call (e.g., “Patient in 402 has a heart rate of 140”).
- Background: Provide context, such as the admitting diagnosis and relevant medical history.
- Assessment: Give your professional opinion on what you believe is happening currently.
- Recommendation: Suggest a specific intervention, like an EKG or a stat lab draw.
- #8: Prioritize a four-patient assignment independently during morning shift changes.
- Review the acuity of each patient and identify who is the most unstable or has time-sensitive meds.
- Create a “brain sheet” that highlights the top priority task for each hour of the 12-hour shift.
- Delegate appropriate tasks (like vitals or hygiene) to the UAP to focus on nursing-level assessments.
- #9: Analyze lab results (CBC/BMP) and explain their clinical significance to the preceptor.
- Identify “critical values” and understand the facility’s protocol for reporting them to the provider.
- Connect electrolyte imbalances, such as low potassium, to potential cardiac dysrhythmias.
- Discuss how the patient’s current medications might be influencing their lab trends.
- #10: Anticipate the needs of a post-operative patient before they return from the PACU.
- Set up the room with necessary equipment: suction, oxygen, and extra pillows for splinting.
- Prepare the post-op orders and ensure pain medication is available for administration upon arrival.
- Review the surgical report to anticipate potential complications specific to the procedure.
Communication and Collaborative Leadership Goals
- #11: Lead a multidisciplinary care coordination meeting for a complex discharge.
- Collaborate with social workers and physical therapists to determine the safest discharge destination.
- Identify barriers to care at home, such as stairs or lack of a primary caregiver.
- Ensure all home health equipment, such as oxygen or a walker, has been ordered and confirmed.
- #12: Effectively educate a patient and their family on new diabetic medication management.
- Use the “teach-back” method to verify the patient understands how to draw up and inject insulin.
- Discuss the signs of hypoglycemia and the “Rule of 15” for emergency glucose management.
- Provide written materials that match the patient’s primary language and literacy level.
- #13: Navigate a difficult conversation with a non-compliant patient using therapeutic techniques.
- Practice active listening and open-ended questions to uncover the root cause of non-compliance.
- Maintain a non-judgmental stance, focusing on the patient’s goals rather than their failures.
- Involve the preceptor or a chaplain if the conflict stems from spiritual or ethical concerns.
- #14: Provide a concise and accurate bedside handoff report for a full patient load.
- Focus on the “active problems” and the plan for the upcoming shift to ensure continuity of care.
- Involve the patient in the report to ensure they are aware of the goals for their recovery.
- Conduct a safety check during handoff, including IV site inspections and pump settings.
- #15: Collaborate with respiratory therapy to manage a patient on high-flow oxygen.
- Understand the settings for Liters per Minute (LPM) and Fraction of Inspired Oxygen (FiO2).
- Assess the patient’s work of breathing and lung sounds before and after therapy adjustments.
- Coordinate oral care and skin assessments around the nasal prongs to prevent pressure injuries.
Advancing through Professionalism and Self-Care (Goals #16 – #31)
- #16: Maintaining a 100% attendance record and arriving 15 minutes early for every shift.
- Use the extra time to look up patient histories before the official handoff begins.
- Demonstrate reliability and commitment to the unit culture by being consistently present.
- Prepare physically and mentally for the shift, ensuring you are well-rested and hydrated.
- #17: Seeking constructive feedback daily and documenting one area for improvement.
- Ask the preceptor at mid-shift: “What is one thing I could do more efficiently right now?”
- Keep a clinical journal to track your growth and the specific lessons learned each day.
- Turn “failures” into learning moments by analyzing what went wrong without self-criticism.
- #18: Participating in a unit-based quality improvement project or committee meeting.
- Identify a common issue on the unit, such as high noise levels at night or frequent call bell use.
- Research evidence-based solutions to present to the unit manager or nurse educator.
- Observe how hospital policies are updated based on clinical data and patient outcomes.
- #19: Demonstrating cultural humility when caring for patients from diverse backgrounds.
- Ask patients about their preferences for dietary needs, modesty, or family involvement in care.
- Utilize a certified medical interpreter rather than family members for all clinical teaching.
- Reflect on personal biases and how they might impact the delivery of equitable healthcare.
- #20: Recognizing personal stress triggers and utilizing one healthy coping mechanism during shift.
- Identify symptoms of “compassion fatigue” or “burnout” during particularly heavy clinical days.
- Practice a 60-second breathing exercise when feeling overwhelmed by high patient acuity.
- Debrief emotional cases with your preceptor to process the stress in a healthy way.
- #21: Developing a “Sunday Reset” routine to prepare for the upcoming clinical week.
- Meal prep healthy lunches and snacks to ensure you have sustained energy during 12-hour shifts.
- Review the pharmacology and pathophysiology related to the patients on your current unit.
- Lay out scrubs and supplies the night before to reduce morning decision fatigue.
- #22: Completing all electronic health record (EHR) charting before the end of the shift.
- Adopt a “chart as you go” philosophy to ensure real-time accuracy and prevent end-of-shift backlog.
- Avoid the use of “copy and paste” to ensure each note accurately reflects the current patient state.
- Perform a final chart audit at 18:00 to ensure all PRN medications and vitals are documented.
- #23: Mastering the interpretation of basic EKG rhythms on a telemetry unit.
- Identify Sinus Rhythm, Bradycardia, Tachycardia, and common arrhythmias like Atrial Fibrillation.
- Understand the clinical implications of a prolonged PR interval or a widened QRS complex.
- Correlate the rhythm on the monitor with the patient’s physical pulse and blood pressure.
- #24: Correcting a peer or self during a “near-miss” to ensure patient safety.
- Speak up immediately if you notice a break in sterile technique or a medication discrepancy.
- Report near-misses through the facility’s incident reporting system to help identify systemic issues.
- Participate in a “root cause analysis” to understand how the error almost occurred.
- #25: Identifying the mechanism of action for the top 10 most common drugs on the unit.
- Create flashcards for medications like Furosemide, Metoprolol, and Enoxaparin.
- Explain how each drug affects the patient’s vital signs and what labs must be checked before administration.
- Differentiate between therapeutic effects and adverse reactions for each medication.
- #26: Managing time effectively to ensure all patient hygiene needs are met by mid-shift.
- Incorporate baths and linen changes into the morning assessment to “cluster” care.
- Delegate hygiene tasks to the UAP early in the shift while maintaining accountability for the outcome.
- Assess for skin breakdown during the hygiene process, focusing on the sacrum and heels.
- #27: Demonstrating proper PPE usage and infection control during isolation precautions.
- Memorize the requirements for Contact, Droplet, and Airborne precautions.
- Perform “donning and doffing” of PPE in the correct sequence to prevent self-contamination.
- Educate family members on why isolation is necessary and how they can stay safe while visiting.
- #28: Utilizing evidence-based practice (EBP) to justify a clinical intervention.
- Look up a unit-specific policy and find the research study that supports that protocol.
- Ask your preceptor: “What does the latest research say about the best way to clean this wound?”
- Share a relevant article from a nursing journal with the staff during a shift huddle.
- #29: Participating in a mock-code or actual emergency response team.
- Understand your role as a student, whether it is performing compressions or recording times.
- Observe the “closed-loop communication” used by the code leader and the team members.
- Attend the “post-code debrief” to learn what went well and what could be improved for next time.
- #30: Developing a professional resume that highlights preceptorship achievements.
- Quantify your experience, such as: “Managed a 4-patient load in an ICU setting under supervision.”
- Include specific certifications earned, such as ACLS or PALS, during your rotation.
- Highlight soft skills like “conflict resolution” and “interdisciplinary collaboration.”
- #31: Successfully completing the final clinical evaluation with “satisfactory” in all domains.
- Review the evaluation tool at the start of the preceptorship to know exactly what is expected.
- Schedule a mid-point evaluation meeting to ensure you are on track to meet all criteria.
- Proactively address any “unsatisfactory” marks by creating a remediation plan with your preceptor.
Managing Medication Safety and Pharmacological Accuracy
Medication errors remain a leading cause of patient harm, making pharmacological mastery a top priority for every student. By setting smart goals for nursing students during preceptorship examples focused on drug administration, you protect your license and your patients. This section compares two primary methods of medication verification to help you choose the safest approach.
Comparison of Verification Workflows
| Feature | Manual Double-Check | Barcode Medication Admin (BCMA) |
| Primary Strength | Human critical thinking | Hard-stop technology alerts |
| Common Failure Point | Interruption/Distraction | Over-reliance on the scanner |
| Speed | Slower, requires two nurses | Faster, independent process |
| Error Prevention | Catches dosing logic errors | Catches “wrong patient” errors |
Navigating the Preceptor-Student Relationship
The dynamic between you and your mentor is the foundation of your learning experience during this final phase of school. Clear communication regarding your smart goals for nursing students during preceptorship examples ensures that your mentor knows exactly how to support your growth. High-quality student research into the “Preceptor-Preceptee” model suggests that proactive students often receive more complex and rewarding assignments.
Techniques for Effective Feedback Integration
- Ask for a “two-minute debrief” after every significant patient intervention.
- Frame your questions around “why” a certain action was taken to understand the clinical logic.
- Acknowledge areas of weakness early to allow your preceptor time to find learning opportunities.
Overcoming the “Fear of Asking”
- Recognize that “I don’t know” is a safe answer that prevents patient harm.
- Keep a small notebook to jot down questions for the end of the shift.
- Value the preceptor’s experience as a living textbook of clinical wisdom.
Documentation and Legal Responsibilities in Nursing
If it wasn’t charted, it wasn’t done; this mantra is the backbone of nursing accountability and legal protection. Developing smart goals for nursing students during preceptorship examples that target documentation will save you from future legal pitfalls. This section outlines the transition from student-level charting to the professional standard of “charting by exception.”
Optimizing Your Electronic Health Record (EHR) Skills
- Use standard medical abbreviations to ensure clarity and professional brevity.
- Chart in real-time or as close to the event as possible to maintain accuracy.
- Double-check that all “required fields” are completed before signing off on a shift.
Career Transition: Moving from Preceptorship to Employment
The end of your preceptorship marks the beginning of your journey as a Registered Nurse, making this the time to synthesize everything you have learned. Reflecting on your smart goals for nursing students during preceptorship examples provides the perfect material for your first professional interviews. You are no longer just a student; you are a prepared professional ready to contribute to the healthcare team.
Leveraging Your Clinical Experience for Your Resume
- Highlight the specific number of patients you managed independently by the end of rotation.
- List technical skills mastered, such as tracheostomy care or chest tube management.
- Mention any unit-specific accolades or positive feedback received from the nursing staff.
Conclusion: Your Roadmap to Nursing Mastery
As you conclude this intensive clinical journey, remember that the habits you formed today will define the nurse you become tomorrow. Master your clinical rotation using smart goals for nursing students during preceptorship examples to refine skills and ensure patient safety. By remaining committed to continuous learning and the SMART framework, you ensure a smooth and successful transition into your new professional life.
Meta Description: Master your clinical rotation using smart goals for nursing students during preceptorship examples to refine skills and ensure patient safety.
Ready to turn your preceptorship successes into a standout professional resume? Trust StudentResearch.net to craft your quality improvement projects and clinical case studies. Visit our platform now to order for specific academic writing services and launch your nursing career!