Table of Contents
ToggleAre you feeling overwhelmed by the transition from textbook theory to the high-stakes environment of the hospital floor? Nursing case studies examples for nursing students act as the essential bridge, transforming abstract medical concepts into the critical thinking skills required to save lives. By engaging with these realistic scenarios, you develop the clinical judgment necessary to navigate complex patient care with confidence and precision.
Why Clinical Case Scenarios are Vital for Modern Nursing Education
Case-based learning is a cornerstone of the nursing curriculum because it mimics the unpredictable nature of healthcare. These nursing case studies examples for nursing students challenge you to prioritize interventions and anticipate complications before they occur. By analyzing these situations, you move beyond rote memorization into the realm of professional clinical reasoning.
Benefits of Practicing with Nursing Case Studies
Practicing with varied scenarios ensures that you are prepared for the diverse patient populations you will encounter during your clinical rotations. It fosters a proactive mindset rather than a reactive one, which is crucial for patient safety.
- Enhanced Critical Thinking: Develops the ability to connect pathophysiology to bedside symptoms.
- NCLEX Preparation: Many board exam questions are formatted as mini-case studies.
- Confidence Building: Reduces anxiety by familiarizing students with “worst-case” scenarios in a safe environment.
- Student Research Integration: High-quality student research indicates that case-based learning significantly improves long-term retention of pharmacological data.
Struggling to bridge the gap between theory and clinical practice? Let StudentResearch.net simplify your journey. Our expert writers deliver high-quality, evidence-based nursing papers that sharpen your critical thinking and boost your grades. Elevate your academic performance today!
How to Analyze a Nursing Case Study Effectively
To get the most out of these examples, you must approach them systematically, much like you would a real patient assessment. Look for “red flags” in the data provided and always prioritize the ABCs (Airway, Breathing, Circulation).
- Read the Subjective Data: Pay attention to what the patient says about their pain or history.
- Evaluate Objective Findings: Analyze vital signs, lab results, and physical exam findings.
- Identify the Nursing Diagnosis: Determine the most pressing human response to the health condition.
#1 Respiratory Distress: A Case of Acute Exacerbation of Asthma
Respiratory issues are among the most common reasons for emergency admissions, making this a foundational scenario for any student. This case focuses on a 12-year-old male presenting with wheezing and increased work of breathing. Immediate recognition of declining respiratory status is the primary goal of this exercise.
Clinical Presentation and Assessment Findings
The patient arrives with a high respiratory rate and visible intercostal retractions. Understanding the difference between “mild distress” and “impending failure” is key to successful nursing intervention.
- Vital Signs: Heart rate 125 bpm, Respiratory rate 34, SpO2 89% on room air.
- Physical Exam: Inspiratory and expiratory wheezes noted in all lung fields; patient is unable to speak in full sentences.
- Patient History: Known history of exercise-induced asthma; missed last two doses of maintenance inhaler.
Immediate Nursing Interventions for Asthma
When a patient is in active respiratory distress, the nurse must act quickly to improve oxygenation and reduce airway inflammation.
- Positioning: Place the patient in High-Fowler’s position to maximize lung expansion.
- Oxygen Therapy: Administer supplemental oxygen via nasal cannula to maintain SpO2 >92%.
- Medication Administration: Prepare for STAT nebulized Albuterol and Ipratropium bromide as ordered.
#2 Cardiovascular Crisis: Managing Unstable Angina in the Elderly
Cardiovascular disease remains a leading cause of morbidity, requiring nurses to be experts in chest pain protocols. In this scenario, a 68-year-old female reports “crushing” substernal chest pain that radiated to her left jaw. This case tests your ability to differentiate between stable and unstable cardiac events.
Interpreting Diagnostic Data for Chest Pain
Diagnostic tests like EKGs and Troponin levels provide the objective data needed to confirm a myocardial infarction. As a student, you must learn to correlate these results with the patient’s clinical “picture.”
- EKG Findings: ST-segment depression in leads II, III, and aVF.
- Laboratory Values: Initial Troponin I is slightly elevated, suggesting myocardial strain.
- Risk Factors: History of hypertension, hyperlipidemia, and a sedentary lifestyle.
Comparison of Cardiac Interventions
Effective management often involves a combination of pharmacological and lifestyle interventions. The following table compares common medications used in cardiac crises.
| Medication | Mechanism of Action | Primary Nursing Consideration |
| Nitroglycerin | Vasodilator; reduces preload and afterload | Monitor for severe hypotension and headache |
| Aspirin | Antiplatelet; prevents clot enlargement | Check for history of GI bleeding or allergies |
| Beta-Blockers | Reduces heart rate and myocardial oxygen demand | Assess apical pulse; hold if HR < 60 bpm |
| Morphine | Analgesic and vasodilator; reduces anxiety | Monitor for respiratory depression |
#3 Endocrine Emergencies: Hyperglycemic Hyperosmolar State (HHS)
Endocrine disorders, particularly Diabetes Mellitus, often lead to complex metabolic crises that require meticulous fluid management. This case involves an 80-year-old resident of a long-term care facility found lethargic with extreme dehydration. It highlights the differences between DKA (common in Type 1) and HHS (common in Type 2).
Assessment of the Dehydrated Diabetic Patient
The hallmark of HHS is profound hyperglycemia without significant ketoacidosis. Students must be vigilant about neurological changes resulting from high serum osmolality.
- Blood Glucose: Results show a “High” reading on the glucometer (>600 mg/dL).
- Neurological Status: Patient is oriented only to person; Glasgow Coma Scale (GCS) score of 12.
- Skin Turgor: Poor skin turgor and dry mucous membranes indicate severe fluid volume deficit.
H4: Nursing Priorities in Metabolic alkalosis/Acidosis
While HHS focuses on fluid replacement, the nurse must ensure the transition is gradual to avoid cerebral edema.
- Fluid Resuscitation: Start IV Normal Saline (0.9% NaCl) as the initial bolus per provider orders.
- Insulin Therapy: Initiate a low-dose insulin infusion once fluid replacement is underway.
- Electrolyte Monitoring: Pay close attention to Potassium levels, as insulin will shift K+ back into the cells.
#4 Post-Operative Complications: Identifying Deep Vein Thrombosis (DVT)
Surgical recovery is a high-risk period for venous thromboembolism, making vigilant assessment a nursing priority. This case follows a 55-year-old patient three days after a total hip arthroplasty who complains of calf tenderness. This nursing case studies examples for nursing students scenario emphasizes prevention and early detection.
H3: Signs and Symptoms of DVT in Surgical Patients
A nurse’s physical assessment is often the first line of defense against a DVT progressing to a pulmonary embolism. Early signs can be subtle, so comparative assessment of the limbs is vital.
- Unilateral Edema: The left calf is 3 cm larger in circumference than the right calf.
- Localized Warmth: The affected area feels warm to the touch and appears erythematous.
- Pain Level: The patient rates pain as a 6/10, localized to the posterior lower leg.
DVT Prevention vs. Treatment
The goal of nursing care is to move from prevention to active management once a clot is suspected.
| Nursing Action | Rationale |
| Ambulation | Increases venous return and prevents stasis (Pre-clot) |
| Bed Rest | Prevents dislodgement of a suspected clot (Post-clot) |
| Sequential Compression Devices | Mimics the muscle pump to move blood (Pre-clot) |
| Anticoagulation (Heparin) | Prevents the clot from growing larger (Post-clot) |
#5 Neurological Assessment: Recognizing Acute Ischemic Stroke
Time is brain when dealing with a stroke, necessitating a rapid and accurate neurological evaluation. This case involves a 72-year-old male who developed sudden right-sided weakness and facial drooping while eating breakfast. Learning the “FAST” acronym through nursing case studies examples for nursing students saves critical minutes in the clinical setting.
The NIH Stroke Scale in Nursing Practice
The NIH Stroke Scale (NIHSS) is a standardized tool used by nurses to quantify the severity of a stroke. Mastering this tool allows for objective communication between the nursing staff and the neurology team.
- Level of Consciousness: Assessing if the patient can follow commands and answer basic questions.
- Visual Fields: Testing for hemianopsia (loss of half of the field of vision).
- Motor Function: Grading the drift in arms and legs when held against gravity.
Is the pressure of NCLEX-style questions weighing you down? StudentResearch.net provides comprehensive study guides and custom academic support tailored to nursing curriculum standards. We help you master complex pathophysiology so you can approach your exams with total confidence.
Nursing Care During Fibrinolytic Therapy
If the patient is a candidate for tPA (Alteplase), the nurse’s role becomes focused on intensive monitoring for hemorrhage.
- Blood Pressure Control: Maintain BP below 180/105 mmHg to prevent intracranial bleeding.
- Bleeding Precautions: Avoid invasive procedures (IV starts, foley insertion) for 24 hours post-infusion.
- Frequent Neuro Checks: Perform assessments every 15 minutes during the infusion.
#6 Pediatric Care: Managing Dehydration in Gastroenteritis
Pediatric patients are highly susceptible to fluid shifts, making dehydration a frequent and serious clinical concern. This case examines a 4-year-old female with a 48-hour history of vomiting and diarrhea. Using student research methods to track weight loss is the most accurate way to determine the degree of dehydration.
Assessing Fluid Deficit in Children
Children do not always show typical adult signs of dehydration until they are severely compromised. Nurses must look for behavioral cues and physiological markers specific to the pediatric population.
- Tear Production: Absence of tears when crying is a significant indicator of fluid loss.
- Urine Output: Weighing diapers to ensure at least 1-2 mL/kg/hr of output.
- Fontanels: In younger infants, a sunken fontanel suggests moderate to severe dehydration.
Rehydration Strategies: Oral vs. IV
The choice between oral rehydration therapy (ORT) and intravenous fluids depends on the severity of the symptoms and the child’s ability to tolerate fluids.
- Oral Rehydration: Preferred for mild dehydration; involves small, frequent sips of Pedialyte.
- IV Bolus: Necessary for severe dehydration; typically 20 mL/kg of an isotonic crystalloid.
- Education: Teaching parents how to monitor for worsening signs at home.
#7 Mental Health Nursing: Supporting a Patient with Major Depressive Disorder
Psychiatric nursing requires a unique set of communication skills and a high level of empathy. In this case, a 22-year-old university student is admitted for suicidal ideation and self-neglect. This scenario focuses on the therapeutic relationship and safety planning within a behavioral health unit.
Therapeutic Communication Techniques
The way a nurse speaks to a patient in crisis can significantly impact the patient’s willingness to engage in treatment. Avoiding “why” questions and using open-ended statements are essential strategies.
- Active Listening: Maintaining eye contact and nodding to show understanding.
- Reflecting: “It sounds like you are feeling very hopeless about your future.”
- Silence: Allowing the patient time to process their thoughts and speak when ready.
Ensuring a Safe Environment (Milieu Management)
The safety of the patient is the priority in mental health nursing, requiring constant environmental assessment.
- Search of Belongings: Removing items like shoelaces, belts, or sharp objects upon admission.
- Observation Levels: Implementing 1-to-1 observation if the patient is at high risk for self-harm.
- Environmental Rounds: Checking for “ligature points” or other hazards in the patient’s room.
#8 Geriatric Nursing: Polypharmacy and Fall Risk Management

As the population ages, nurses must become experts in the complexities of geriatric care, specifically the risks associated with multiple medications. This case involves an 85-year-old female with five chronic conditions taking twelve different medications. This nursing case studies examples for nursing students exercise highlights the “prescribing cascade.”
Identifying High-Risk Medications in the Elderly
Certain medications, such as benzodiazepines or antihypertensives, significantly increase the risk of falls in older adults. Nurses play a vital role in medication reconciliation and advocating for “de-prescribing” where appropriate.
- Orthostatic Hypotension: Medications that drop blood pressure upon standing are a major fall trigger.
- Cognitive Impairment: Some medications can cause confusion or “sundowning” in the elderly.
- Drug-Drug Interactions: Assessing how new prescriptions may interact with long-standing medications.
Fall Risk Assessment Tools
Using standardized tools like the Morse Fall Scale helps nurses quantify risk and implement appropriate interventions. Student research has shown that standardized assessments reduce fall rates by 25% in acute care settings.
| Risk Factor | Nursing Intervention |
| History of Falls | Place patient in a room close to the nurses’ station |
| Unsteady Gait | Ensure use of non-slip socks and a walker/cane |
| Urinary Urgency | Implement a scheduled toileting program every 2 hours |
| Visual Impairment | Keep the room well-lit and remove clutter from pathways |
Clinical Simulation: Medication Administration Checklist for Pediatric Asthma
High-acuity respiratory cases require the nurse to maintain a calm demeanor while executing precise medical orders. This simulation provides a framework for administering nebulized medications and intravenous corticosteroids, which are the gold standard for opening constricted airways. By practicing these nursing case studies examples for nursing students, you refine your ability to multitask under pressure while maintaining strict adherence to safety protocols.
Pre-Administration Assessment and Preparation
Before any medication reaches the patient, the nurse must verify the clinical need and the safety of the prescribed dose. In pediatric respiratory cases, weight-based dosing is common, making calculation accuracy a life-saving necessity.
- Verify Patient Identity: Use two institutional identifiers (e.g., full name and date of birth).
- Auscultate Lung Fields: Document the presence of wheezing, diminished breath sounds, or “silent chest.”
- Check Vital Signs: Obtain a baseline Heart Rate (HR) and SpO2.
- Review Allergies: Confirm the patient has no known sensitivities to bronchodilators.
- Student Research Validation: Recent student research highlights that bedside verification of the “Six Rights” reduces medication errors by up to 40%.
Step-by-Step Nebulizer Administration Checklist
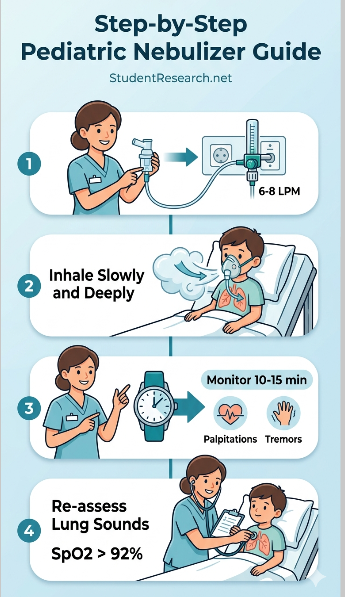
Nebulized Albuterol and Ipratropium (DuoNeb) are often the first-line treatments for acute asthma. Proper technique ensures that the medication reaches the lower airways.
- Assemble the Equipment: Connect the nebulizer cup to the oxygen or compressed air source.
- Set the Flow Rate: Adjust the flow meter to 6–8 liters per minute (LPM).
- Patient Positioning: Ensure the patient is sitting upright (High-Fowler’s).
- Coaching the Patient: Instruct the child to take slow, deep breaths through their mouth.
- Monitor for Side Effects: Observe for tremors, palpitations, or increased anxiety.
- Post-Treatment Assessment: Re-assess lung sounds and work of breathing immediately.
Intravenous Corticosteroid Administration (Methylprednisolone)
While bronchodilators address immediate bronchospasm, corticosteroids are essential for reducing the underlying airway inflammation.
- Verify IV Patency: Flush the peripheral IV line with Normal Saline to ensure it is “flushing well.”
- Dilution and Compatibility: Check the drug manual for dilution requirements and compatibility.
- Administration Rate: Give the medication slowly (usually over 3–5 minutes).
- Document Response: Record the time of administration and clinical status.
Master Clinical Judgment with Nursing Case Studies Examples for Nursing Students
Integrating these nursing case studies examples for nursing students into your daily study routine is the most effective way to prepare for the realities of the nursing profession. By consistently applying the nursing process to these scenarios, you sharpen your intuition and ensure that your care is always evidence-based and patient-centered.
Nursing case studies examples for nursing students provide essential clinical practice, helping learners apply theoretical knowledge to real-world patient care scenarios for better outcomes.
Metadescription: Master clinical judgment with 8 nursing case studies examples for nursing students. Explore respiratory, cardiac, and pediatric care to improve outcomes.
Need a flawlessly researched paper without the midnight stress? StudentResearch.net is your premier partner for nursing excellence. Don’t let deadlines overwhelm you; click here to order for specific academic writing services and secure your future success now!