Table of Contents
ToggleMeta Description: Discover how mathematics for nursing students works — from drug calculations to IV drips — in this complete, confidence-building guide.
Why Nursing Math Could Save a Life — Including Your Patient’s
Picture this: it’s 2 a.m., a patient’s condition is deteriorating fast, and the physician has just ordered an urgent IV medication. Your hands are steady. Your mind is clear. Why? Because you know your nursing math cold.
Mathematics for nursing students is not just an academic hurdle — it is a clinical lifeline. Every dose calculated incorrectly, every IV drip rate misread, or every unit conversion fumbled carries a real-world consequence that no textbook grade can reverse. Research from the Institute for Safe Medication Practices consistently identifies calculation errors as among the top causes of preventable medication harm in healthcare settings. If you are a nursing student wondering whether all those fractions and formulas are truly necessary, the answer — without hesitation — is yes.
This blog walks you through 12 carefully structured sections covering every core area of nursing mathematics, from foundational arithmetic to advanced pharmacology calculations. Whether you are just beginning your clinical rotations or refreshing your skills before NCLEX, this guide is designed to make nursing math logical, manageable, and even empowering.
Understanding Why Math Is Non-Negotiable in Nursing Practice
The Real-World Stakes of Nursing Mathematics for Patient Safety
Nursing is one of the few professions where a mathematical error is not just a wrong answer on paper — it is a potential harm to a living person. Understanding the gravity of this responsibility is the first step every nursing student must take.
- Medication errors account for approximately 1 in 5 adverse events in hospital settings globally (WHO, 2023)
- Over 40% of medication errors are linked to incorrect dose calculations, according to a 2022 systematic review in the Journal of Nursing Education
- Student research published in Nurse Education Today found that nursing students who received structured math training reduced calculation errors by 62%
- Errors are most common during high-pressure, time-sensitive clinical moments — exactly when math fluency matters most
How Mathematics for Nursing Students Differs from General Math
Nursing math is applied, contextual, and consequence-driven, which makes it unique from classroom arithmetic.
- It integrates units, patient weight, concentration, and time simultaneously
- Unlike abstract algebra, every variable represents a real clinical element
- Errors of omission (forgetting to account for a variable) are as dangerous as errors of commission
- The goal is not speed alone — it is accuracy under pressure
Struggling with nursing calculations on your assignment? Let the experts at StudentResearch.net handle the heavy lifting. From drug dosage papers to clinical case studies, we deliver precise, professionally written nursing academic content — on time, every time.
Core Arithmetic Skills Every Nursing Student Must Refresh
Fractions, Decimals, and Percentages in Drug Dosage Calculation
The foundation of mathematics for nursing students begins with operations most people learned in middle school — but must now apply with clinical precision.
- Fractions are used to express partial doses and medication concentrations
- Decimals appear in nearly every drug label, weight-based calculation, and lab value
- Percentages are critical for IV solution concentrations (e.g., 0.9% Normal Saline, 5% Dextrose)
- A misplaced decimal point — moving 1.0 mg to 10 mg — represents a 10-fold overdose
Common Decimal Errors in Nursing Practice
- Trailing zeros (writing 1.0 instead of 1) — banned by The Joint Commission
- Leading zeros omitted (writing .5 instead of 0.5)
- Rounding errors when carrying decimals beyond the second place
- Errors in unit conversion when shifting between mg, mcg, and g
Ratios and Proportions as a Foundational Nursing Math Tool
- The ratio-proportion method is one of the most universally taught approaches to drug calculation
- It expresses the relationship between what you have and what you need
- Formula: Have/Need = Known quantity/Unknown quantity
- Particularly effective for students who are new to dimensional analysis
Mastering the Metric System and Unit Conversions
Why Unit Conversions Are Critical in Nursing Mathematics
Mathematics for nursing students demands fluency in the metric system because nearly all medications and clinical measurements use metric units.
- Medications are ordered in mg, mcg, g, mEq, and units
- Body weight is recorded in kilograms for dose calculations
- Fluid volumes are measured in mL and L
- Failure to convert between units correctly is one of the most cited causes of student-level medication errors
Essential Metric Conversions Every Nursing Student Must Memorize
| Unit From | Unit To | Conversion Factor |
|---|---|---|
| 1 gram (g) | milligrams (mg) | × 1,000 |
| 1 milligram (mg) | micrograms (mcg) | × 1,000 |
| 1 kilogram (kg) | pounds (lb) | × 2.2 |
| 1 liter (L) | milliliters (mL) | × 1,000 |
| 1 teaspoon (tsp) | milliliters (mL) | × 5 |
| 1 tablespoon (tbsp) | milliliters (mL) | × 15 |
Memory Tricks for Unit Conversions
- Use the mnemonic “King Henry Died By Drinking Cold Milk” (Kilo, Hecto, Deca, Base, Deci, Centi, Milli)
- Color-code conversion charts by category: weight, volume, length
- Practice conversions daily using flashcard apps like Anki
- Apply conversions in clinical context: “If a child weighs 44 lbs, what is the weight in kg?” (Answer: 20 kg)
The Three Primary Drug Calculation Methods Explained
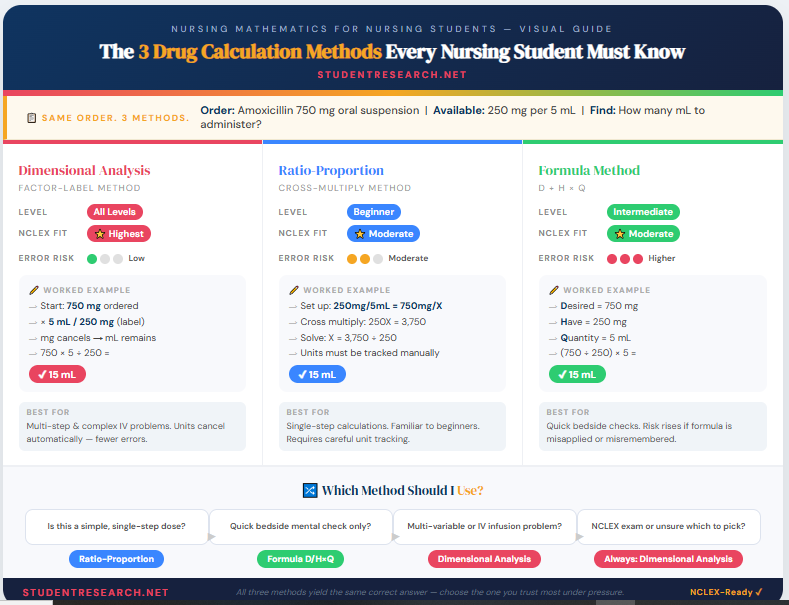
Dimensional Analysis — The Most Recommended Method for Nursing Students
Dimensional analysis (also called the factor-label method) is widely endorsed in nursing education because it reduces multi-step errors into a single, trackable equation.
- Units cancel across the equation, leaving only the desired unit
- Works for simple doses and complex multi-variable IV problems
- Reduces reliance on memorized formulas
- Student research consistently shows higher accuracy rates with dimensional analysis compared to ratio-proportion alone
Step-by-Step Dimensional Analysis Framework
- Step 1: Identify what you want to find (e.g., mL/hr)
- Step 2: Start with the ordered dose as your first fraction
- Step 3: Add conversion fractions so units cancel progressively
- Step 4: Multiply across the numerators, divide by denominators
- Step 5: Confirm the remaining unit matches your goal unit
Ratio-Proportion vs. Formula Method — A Side-by-Side Comparison
| Feature | Ratio-Proportion | Formula Method (D/H × Q) | Dimensional Analysis |
|---|---|---|---|
| Best for | Single-step calculations | Quick bedside calculations | Multi-step/complex problems |
| Error risk | Moderate | Higher (formula misapplication) | Lower |
| Recommended level | Beginner | Intermediate | All levels |
| NCLEX alignment | Moderate | Moderate | High |
| Unit tracking | Manual | Manual | Built-in |
The Formula Method — D/H × Q Simplified
- D = Desired dose (what is ordered)
- H = Have (what is on hand)
- Q = Quantity (vehicle — tablet, mL, etc.)
- Example: Order is 500 mg; on hand is 250 mg/tablet → (500/250) × 1 = 2 tablets
Oral Medication Calculations Made Simple
Calculating Tablets, Capsules, and Liquid Oral Doses
Oral medication calculations are among the first clinical math skills nursing students encounter during patient care simulations.
- Tablets are calculated using the formula method or dimensional analysis
- Scored tablets may be split; unscored and extended-release tablets must never be split
- Liquid oral medications are measured in mL using calibrated oral syringes
- Always double-check the concentration label: mg/mL vs. mg/5mL are fundamentally different
Oral Liquid Dose Calculation Example Breakdown
- Order: Amoxicillin 375 mg oral suspension
- Available: 250 mg per 5 mL
- Calculation: (375 ÷ 250) × 5 mL = 7.5 mL
- Clinical check: Is 7.5 mL a reasonable oral volume? Yes — typical range is 5–30 mL
Pediatric Oral Dose Calculations — Weight-Based Nursing Math
- Pediatric doses are almost always calculated per kilogram of body weight
- Orders are written as mg/kg/day or mg/kg/dose
- Always verify the calculated dose falls within the safe dose range from drug references
- Mathematics for nursing students includes comparing calculated dose against published therapeutic ranges
Parenteral and Injectable Medication Calculations
Calculating Doses for Intramuscular and Subcutaneous Injections
Parenteral calculations require the same formula skills as oral dosing but carry higher stakes due to the invasive route of administration.
- IM injections typically range from 0.5 to 3 mL per site
- Subcutaneous injections are usually 0.5 to 1 mL
- Exceeding volume limits causes tissue damage regardless of calculation accuracy
- Insulin and heparin are high-alert medications requiring independent double-checks
Insulin Calculation Safety Points
- Insulin is measured in units, not milligrams
- Always use an insulin syringe calibrated in units (U-100 most common)
- Never use a standard 1 mL syringe for insulin without unit conversion
- Basal vs. bolus insulin orders require separate calculation pathways
Reconstitution Calculations for Powdered Injectable Medications
- Many antibiotics come in powder form requiring reconstitution with sterile water or saline
- The label specifies how many mL of diluent to add and the resulting concentration
- After reconstitution: apply standard formula to calculate volume to withdraw
- Record date, time, and concentration on the vial after reconstitution
Intravenous Flow Rate Calculations — A Nursing Student Essential
Understanding IV Drip Rates, mL/hr, and Drop Factors
IV flow rate calculations are perhaps the most critical area of mathematics for nursing students entering clinical practice.
- mL/hr is used for electronic infusion pumps (most common in modern hospitals)
- Drops per minute (gtt/min) is used when manual gravity drips are employed
- Drop factor (gtt/mL) is printed on every IV tubing package (typically 10, 15, 20, or 60 gtt/mL)
- Formula: Flow rate (gtt/min) = Volume (mL) ÷ Time (min) × Drop factor
IV Flow Rate Calculation — Worked Example
- Order: Infuse 1,000 mL NS over 8 hours via gravity drip; tubing = 20 gtt/mL
- Step 1: Convert hours to minutes: 8 × 60 = 480 minutes
- Step 2: Calculate: (1,000 ÷ 480) × 20 = 41.7 → round to 42 gtt/min
- Clinical check: Count drops for 15 seconds (target = ~10–11 drops) and multiply by 4
Continuous IV Medication Infusion Rate Calculations
- Many critical care medications (dopamine, heparin, insulin drips) are delivered as continuous infusions
- Orders are written in mcg/kg/min or units/hr — requiring multi-step dimensional analysis
- Student research in critical care simulation labs shows these calculation types have the highest error rates among nursing students
- Always calculate, then verify with a second nurse per institutional protocol
Intravenous Piggyback (IVPB) and Intermittent Infusion Calculations
IVPB Medication Administration and Rate Calculation
IVPB medications are secondary infusions — antibiotics, electrolytes, and analgesics most commonly — delivered over a defined window.
- Common infusion times: 15, 30, 60, or 90 minutes
- Always calculate mL/hr from total volume and infusion time
- Example: Vancomycin 500 mg in 100 mL, infuse over 60 min → 100 mL/hr
- Maximum infusion rates exist for certain medications (e.g., vancomycin ≤ 10 mg/min to prevent Red Man Syndrome)
Calculating Infusion Time and Volume Remaining
- Formula: Infusion time (hr) = Volume ordered (mL) ÷ Flow rate (mL/hr)
- Knowing how to calculate time remaining helps with scheduling the next dose
- Critical for antibiotics given on timed intervals (q6h, q8h, q12h)
- Nursing students should practice documenting start time, expected completion time, and next-dose window
Heparin and Critical Care Drip Calculations
Heparin Infusion Calculations — A High-Alert Medication Priority
Heparin is among the most frequently implicated medications in serious dose errors, making it a central focus in mathematics for nursing students preparing for acute care settings.
- Heparin is ordered in units/hr based on weight-based protocols (units/kg/hr)
- Must calculate: total units/hr → then mL/hr from available concentration
- Continuous monitoring of aPTT guides dose titration (a math-inclusive nursing skill)
- Never estimate or round liberally — heparin errors can cause fatal hemorrhage
Heparin Drip Calculation — Step-by-Step
- Order: Heparin infusion at 18 units/kg/hr; patient weighs 80 kg
- Step 1: 18 × 80 = 1,440 units/hr
- Step 2: Available: 25,000 units in 250 mL NS = 100 units/mL
- Step 3: 1,440 ÷ 100 = 14.4 mL/hr — program the pump to 14.4 mL/hr
Other Critical Care Infusion Calculations Nursing Students Must Know
| Medication | Ordered As | Key Calculation Step |
|---|---|---|
| Dopamine | mcg/kg/min | Convert to mL/hr using concentration |
| Norepinephrine | mcg/min | Calculate mL/hr from mcg/mL concentration |
| Regular Insulin (drip) | units/hr | Use concentration (units/mL) to find mL/hr |
| Heparin | units/kg/hr | Weight-based then concentration conversion |
| Magnesium Sulfate | g/hr | Convert g to mg, then use mL/hr |
Pediatric and Obstetric Nursing Calculations
Weight-Based Dosing in Pediatric Nursing Mathematics
Pediatric nursing mathematics demands an additional layer of scrutiny because children cannot self-report adverse effects as clearly as adults.
- All pediatric doses are calculated in mg/kg or mcg/kg/min
- After calculating the dose, always compare to the maximum safe dose in references like Tarascon or Lexicomp
- Never assume an adult dose is safe at a reduced fraction without consulting a pediatric reference
- Student research in pediatric simulation settings confirms that most student errors occur at the verification step, not the calculation step
Pediatric Safe Dose Range Verification Steps
- Step 1: Calculate dose based on weight (mg/kg)
- Step 2: Look up the therapeutic range: minimum and maximum mg/kg/dose or mg/kg/day
- Step 3: Confirm calculated dose falls between the minimum and maximum
- Step 4: If outside range — do NOT administer; contact prescriber immediately
Obstetric Infusion Calculations — Pitocin and Magnesium Sulfate
- Oxytocin (Pitocin) is titrated in milliunits/minute (mU/min) — a unit unique to obstetrics
- Conversion: 1 unit = 1,000 milliunits
- Magnesium sulfate (used for preeclampsia) has a narrow therapeutic window — toxicity monitoring is mathematical as well as clinical
- Both medications require continuous nurse calculation and pump verification throughout labor
NCLEX-Style Math Questions and Test-Taking Strategies How Mathematics for Nursing Students Appears on the NCLEX-RN
The NCLEX includes calculation questions in both traditional and next-generation formats, making math fluency directly tied to licensure success.
- Calculation questions are typically presented as fill-in-the-blank (not multiple choice)
- You are provided with an on-screen calculator — but setup errors still occur
- The NCLEX tests dimensional analysis thinking, not just formula recall
- Common tested topics: IV flow rates, safe dose range, unit conversions, weight-based dosing
Proven NCLEX Math Preparation Strategies for Nursing Students
- Practice daily — 10–15 calculation problems per day beginning 90 days before the exam
- Use NCLEX prep platforms (UWorld, BoardVitals, Kaplan) that include calculation question banks
- Review rationales for both correct and incorrect answers to understand the why
- Time yourself: NCLEX allows approximately 1.5 minutes per question on average
Most Common NCLEX Calculation Question Types
- IV drip rate and flow rate problems
- Weight-based safe dose range questions
- Oral tablet and liquid dosing
- Unit conversion problems (especially mcg ↔ mg ↔ g)
- Reconstitution calculations
- Heparin and insulin administration problems
Conclusion — Building Lasting Math Confidence as a Nursing Student
From Classroom Formulas to Clinical Confidence — Your Mathematics Journey
Discover how mathematics for nursing students transforms from an anxiety-inducing course requirement into one of your most powerful clinical tools — one practiced dose at a time. If there is a single theme woven through every section of this guide, it is this: nursing math is not about being a mathematician. It is about being a safe, dependable, and precise practitioner who can be trusted with someone’s life at 2 a.m. Every formula, every conversion, every drip rate calculation you master adds one more layer of protection between your patient and preventable harm.
The 12 strategies covered in this guide — from core arithmetic and metric conversions, through oral and parenteral calculations, IV flow rates, heparin drips, pediatric dosing, and NCLEX preparation — represent the full landscape of nursing mathematics you will encounter from student rotations through your first years of professional practice. Student research across nursing education programs consistently confirms that students who approach math systematically, practice regularly, and seek to understand the why behind each formula perform better clinically and report higher confidence levels at the bedside.
Your mathematical competence is not separate from your clinical competence — it is your clinical competence, expressed in numbers.
Actionable Next Steps to Strengthen Your Nursing Math Skills Today
- Review one calculation method per week — rotate between dimensional analysis, ratio-proportion, and formula method
- Use simulation labs to practice calculations in real clinical scenarios before patient contact
- Build a personal formula reference sheet laminated for clinical rotations
- Track your errors — each mistake is a data point, not a verdict on your abilities
- Connect with peers — group problem-solving mirrors the collaborative double-check culture of real nursing units
- Revisit this guide before each new clinical placement or exam block
Mathematics for nursing students is a skill — and like every skill, it grows stronger every time you use it. Keep calculating. Keep questioning. Keep caring enough to get it right.
Deadlines piling up faster than IV drip calculations? StudentResearch.net is your trusted academic partner. Our nursing-specialist writers deliver thoroughly researched, plagiarism-free papers tailored to your curriculum — so you can focus on mastering clinical skills that save lives